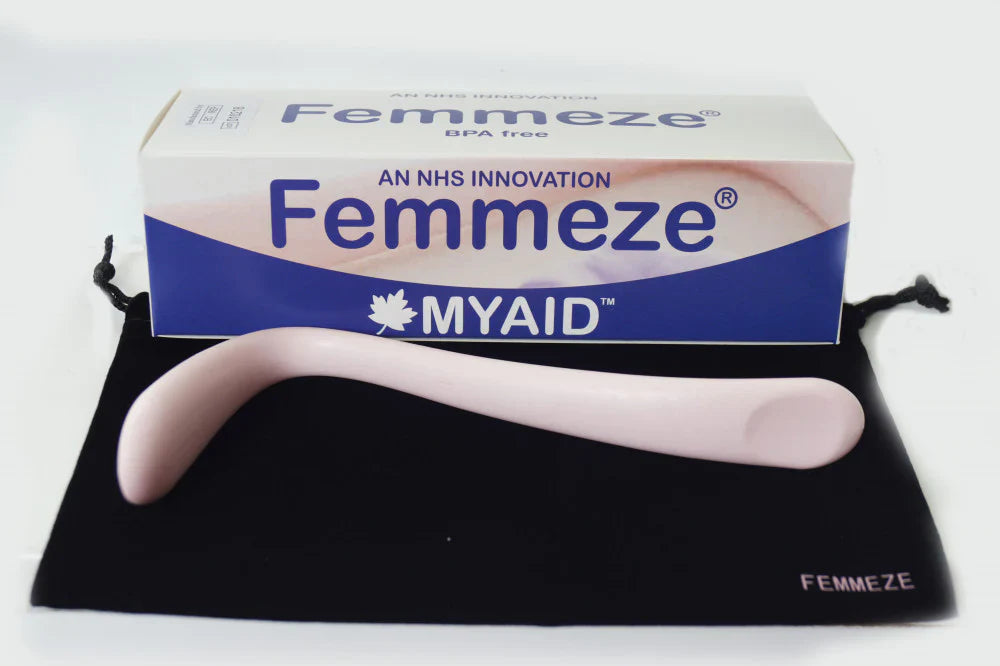
If you or a patient has been diagnosed with rectocele, also known as posterior vaginal wall prolapse, you may have experienced difficulty with bowel movements, a sensation of incomplete evacuation, or the need to apply pressure during defecation. These functional symptoms often lead women to seek conservative options before surgical repair is considered.
The FEMMEZE Rectocele Vaginal Device is a tool designed to provide structured vaginal support during bowel movements for women practicing vaginal splinting. This article explains what it is, how it works, and where it fits in rectocele symptom management.
What Is a Rectocele?
Rectocele is a type of pelvic organ prolapse in which the rectal wall protrudes into the posterior vaginal canal due to weakening of supporting muscles and connective tissues.
According to the National Institute of Diabetes and Digestive and Kidney Diseases:
-
Pelvic floor disorders affect nearly 1 in 4 women in the U.S.
-
The incidence of prolapse increases with age and childbirth history.
Symptoms of rectocele can include:
-
Straining during bowel movements
-
Incomplete evacuation
-
Pelvic pressure
-
Vaginal bulge or pressure sensation
The American College of Obstetricians and Gynecologists emphasizes that treatment planning is primarily driven by symptom severity and patient goals.
What Is Vaginal Splinting?
Vaginal splinting is a technique in which a woman applies digital pressure inside the vagina to support the rectal wall and facilitate stool progression. While this can be effective, many seek alternatives that are more structured, ergonomically designed, and hygienic.
What Is the FEMMEZE Rectocele Vaginal Device?
The FEMMEZE Rectocele Vaginal Device is a single-use vaginal support tool developed to assist women with rectocele-related bowel difficulties.
Instead of using a finger for vaginal splinting, which can be inconsistent or uncomfortable, the device provides a structured, anatomical support surface that helps women apply posterior pressure during defecation.
The FEMMEZE device is intended for symptomatic support only, not for repairing or curing rectocele.
How the FEMMEZE Device Works
The device is designed for easy insertion and handling:
-
Insert the device vaginally before a bowel movement.
-
Apply gentle posterior pressure to help stool evacuation.
-
Reduce reliance on digital splinting by using a structured support surface.
-
Discard after single use for hygiene.
This structured method may reduce discomfort and provide more consistent support compared with manual finger pressure.
Who May Benefit from FEMMEZE?
The FEMMEZE Rectocele Vaginal Device may be considered for women who:
-
Have a rectocele with obstructed defecation symptoms
-
Routinely perform vaginal splinting
-
Prefer non-surgical management of symptoms
-
Seek a more ergonomic alternative to manual support during bowel movements
It is generally recommended to discuss use with a healthcare provider for proper guidance and symptom assessment.
Where Does FEMMEZE Fit in Conservative Rectocele Care?
U.S. clinical guidance encourages an individualized approach to rectocele management:
-
The American Urogynecologic Society and American College of Obstetricians and Gynecologists support conservative therapies before considering surgery when appropriate.
-
These include pelvic floor muscle training, bowel habit optimization, pessary use, and symptom-targeted tools.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, lifestyle and functional therapies are important components in addressing defecatory dysfunction.
Within this context, the FEMMEZE device may be used as part of a non-surgical symptom management strategy.
Advantages of a Structured Rectocele Support Device
Compared with traditional manual splinting, a vaginal support device provides:
-
Consistent anatomical support
-
Ergonomic handling
-
Reduced direct finger contact
-
Single-use hygiene convenience
Women often find that structured devices offer a more comfortable user experience.
Important Notes Before Use
-
The FEMMEZE device is supportive, not therapeutic.
-
It does not repair rectocele or change pelvic anatomy.
-
Clinical evaluation is recommended to rule out other causes of bowel dysfunction.
Women with severe symptoms, pain, bleeding, or urinary issues should consult a clinician for proper assessment.
Frequently Asked Questions
Can FEMMEZE replace pelvic floor therapy?
No. Pelvic floor physical therapy is a foundational intervention. Devices like FEMMEZE may complement therapy but do not replace clinical rehabilitation.
What is the FEMMEZE rectocele device used for?
The FEMMEZE rectocele vaginal device is designed to provide structured vaginal support during bowel movements for women experiencing obstructed defecation due to posterior vaginal wall prolapse (rectocele). It assists with symptom management but does not treat or cure prolapse.
How does a rectocele support device work?
A rectocele support device is inserted vaginally to apply gentle posterior pressure against the rectal wall. This may help improve stool evacuation in women who otherwise perform manual vaginal splinting.
Who may benefit from using a vaginal splinting device?
Women who:
-
Experience incomplete bowel emptying
-
Perform digital vaginal splinting
-
Prefer non-surgical rectocele management
-
Have mild to moderate posterior vaginal wall prolapse
Clinical evaluation is recommended before starting any device use.
What are common symptoms of rectocele?
Common symptoms include:
-
Vaginal bulging sensation
-
Straining during bowel movements
-
Incomplete stool evacuation
-
Pelvic pressure
-
Need for manual vaginal splinting
If symptoms worsen, medical consultation is recommended.
U.S. Clinical Guidance on Rectocele Symptom Management
U.S. evidence-based sources emphasize symptom-guided management:
-
The American College of Obstetricians and Gynecologists states that conservative therapies can be first-line for many women.
-
The American Urogynecologic Society supports individualized treatment.
-
The National Institute of Diabetes and Digestive and Kidney Diseases highlights the importance of bowel habit optimization.
These sources guide clinicians and patients in choosing appropriate strategies based on symptoms.
Conclusion
The FEMMEZE Rectocele Vaginal Device offers a structured option for women seeking symptom relief from rectocele-related bowel difficulties. When used thoughtfully within a broader conservative management plan, it may help reduce reliance on manual vaginal splinting and improve comfort during bowel movements.
Women experiencing symptoms should consult a qualified clinician for individualized care planning.